Chronic constipation affects around 10-15% of the population. In general, the prevalence of constipation in North America has been quoted as 1.9% to 27.2%.
The Rome Foundation was established in 1991, and they released the Rome III criteria in 2006 that standardizes and defines constipation. Chronic constipation is defined as experiencing at least two of the following while making a bowel movement. Straining during defecation, lumpy or hard stools, sensation of incomplete evacuation, sensation of anorectal obstruction/blockage, need for manual maneuvers to facilitate defecation and fewer than 3 defecations per week. For constipation to be defined as chronic a patient must be symptomatic for at least 6 months with applicable criteria for the previous 3 months.
Identifying constipation
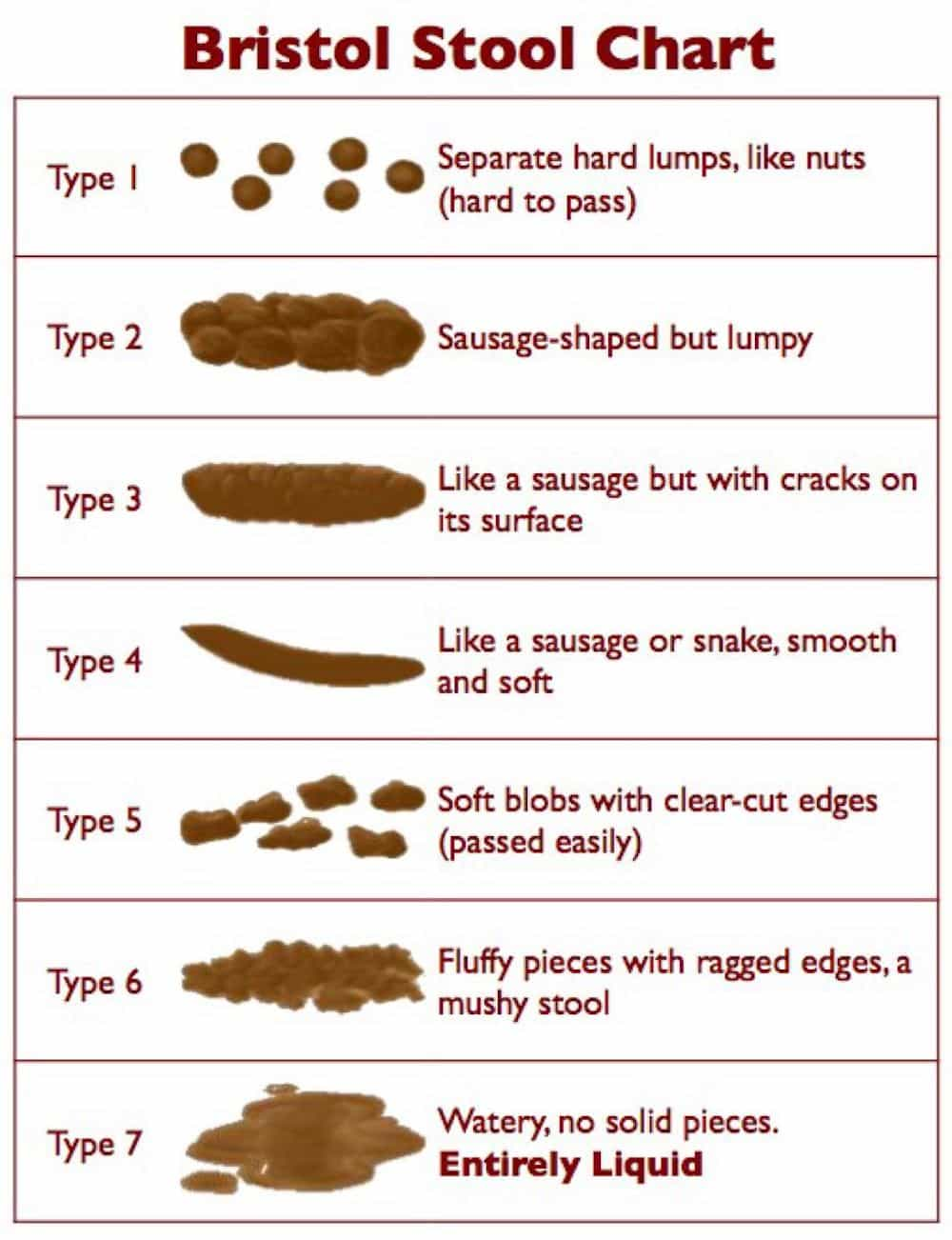
The Bristol Stool Form Scale (BSFS), developed by Ken Heaton, MD from the University of Bristol, is a tool that assesses stool consistency based on seven types. If yours is type one or two, hard and lumpy – you’re probably constipated. The ideal stool is generally type three or four, easy to pass, without being too watery. Types five, six and seven tend to signify loose or watery stool (diarrhea).
What to do if you suffer from Constipation:
For many healthy adults, constipation can be caused by inadequate hydration, a low-fiber diet, and inactivity. In addition, never ignore the urge to defecate. It can mess up your process of elimination for weeks.
So, why is hydration so important? Water is needed for vital daily processes and our bodies control the amount of water in our stool. If your body needs water for higher level bodily functions but doesn’t have the amount it needs, it might not allow for enough in your stool. Due to inadequate water in your stool, your bowel movements may harden and then become difficult to pass. As a rule of thumb, for most healthy adults, try to drink 2 liters of water or 8 cups daily. If you don’t like the taste of water, try adding fruit or citrus or opt for a low-calorie or no calorie sparkling water. Needs will also differ depending on your age, height and the amount of physical activity you do daily. To meet your needs, carry around or place a pre-measured container in a bag or in the fridge for daily use.
Next look at the amount of fiber in your diet. Recommendations from the Institute of Medicine suggest that adults should consume 20-35 grams of fiber per day. In reality, the average American’s daily intake of dietary fiber is only 12-18 grams. Fiber is a complex carbohydrate and can be found in fruits, vegetables, whole grains, beans and legumes.
All fiber, is found in either soluble or insoluble forms. It is found in plant foods and is not digested by humans. Soluble, fermentable fiber dissolves in water and gastrointestinal fluids when it enters the stomach and intestines. It is transformed into a gel-like substance and fermented by the gut microbiota in the colon to produce short chain fatty acids (SCFA). SCFAs are a source of energy for colonocytes, and they help to increase intestinal mucosal growth and promote water and sodium absorption. When digested in the colon, it releases gases and a few calories and also slows down or increases transit time. Insoluble fiber is not effectively fermented by the gut microbiota, does not dissolve in water and is left intact as food moves through the gastrointestinal tract. Because it is not digested at all, insoluble fiber is not a source of calories.
Soluble fiber found in beans, oats, flaxseed and oat bran can prevent some dietary cholesterol from being broken down and digested by clearing it from the system. It reduces the risk of cardiovascular disease by not only lowering cholesterol levels but also decreases fat absorption. In people with diabetes, soluble fiber stabilizes blood sugar by slowing down the digestion rate of carbohydrates and prevents spikes in blood sugar. Other examples of soluble fiber include apples, citrus fruits, peas, oatmeal and psyllium.
Insoluble fiber may help to prevent constipation by decreasing transit time and increasing fecal weight. Insoluble fiber sits in the gastrointestinal tract, absorbing fluid and sticking to other byproducts of digestion that are ready to be formed in the stool. Its presence speeds up the movement and processing of waste. Examples of insoluble fiber include prunes, nuts, wheat bran, whole grain breads and vegetables such as cauliflower, green beans and potatoes.
To receive the greatest health benefit, eat a wide variety of high-fiber foods. Aside from normalizing bowel movements, aiding in cardiovascular disease and diabetes, fiber can help with weight management. High-fiber foods are more filling and will keep you full longer. You’ll be less likely to nosh on calorie-dense foods. A word of caution, adding too much fiber too quickly can promote intestinal gas, abdominal bloating and cramping. In addition, fiber breaks down into tiny pieces we call residue and can make constipation worse by blocking your GI tract without enough fluid to push it along. Remember, drink plenty of water – fiber works best when it absorbs plenty of water, making your stool soft, bulky and easy to pass.
Exercise helps constipation by lowering the time it takes food to move through the large intestine. Running, skipping and jumping movements create mechanical assistance to aid with bowel movements. Do some form of physical activity for approximately 30 minutes each day.
What if diet and lifestyle factors don’t work?
If you’re still constipated after gradually adding more fiber, fluid and exercise to you diet and lifestyle, there could be other reasons such as a medical condition or a side effect from some medications.
The elderly often can suffer from constipation due to reduced thirst sensation, immobility, and having to take multiple medications. Women who are pregnant produce more of the hormone progesterone, which might make it more difficult for intestinal muscles to contract. If you are in a low socioeconomic bracket research has shown that food deserts provide inadequate access to fresh fruits and vegetables, and often are filled with fast food chains that mostly offer unhealthy food choices. People suffering from depression could make poor food choices and be on medications that affect bowel motility.
Medications including opiates, anti-depressants, acetaminophen, aspirin, NSAIDs, Iron Supplements, B-blockers, anticholinergics and diuretics can also contribute to constipation. Endocrine and metabolic disorders can affect bowel movement regularity. Diabetes due to lack of insulin can cause high blood sugar levels that lead to diabetic neuropathy, or nerve damage. According to the Mayo Clinic, damage to the nerves controlling the digestive tract can lead to constipation. Hypothyroidism causing a sluggish metabolism slows down your whole digestive system which can cause constipation. Neurological disorders that can interfere with brain-gut signals including dementia, Parkinson’s disease, and spinal cord injuries are also risk factors.
If constipation persists, visit your doctor and seek more diagnostic testing. For meal planning, consult a dietitian.

